iStent Surgery
What is Glaucoma and How is it Treated?
Glaucoma is a chronic disease defined by characteristic optic nerve damage. It is a multifactorial disease with over 300 different anatomic variations and affects over 40,000,000 people worldwide. Glaucoma is a progressive and irreversible disease and in most cases, causes a painless loss of eyesight. Because Glaucoma is oftentimes a symptomless disease, it is also known as “the sneak thief of sight.” Glaucoma may lead to damage to the optic nerve. This damage is commonly caused by a fluid imbalance, or pressure, in the eye, as well as possible changes in the blood flow to the optic nerve. It is well established that lowering the intraocular pressure can slow the process of optic nerve damage. The degree of pressure lowering necessary to prevent optic nerve damage is individualized for each person and each optic nerve. The greater the optic nerve damage, the lower the intraocular pressure that is needed to achieve stability and prevent further optic nerve damage and further visual field loss.
If Dr. Darlington or Dr. McManus has diagnosed you with glaucoma and has informed you that if it is left untreated, you may experience vision loss and eventual blindness. Treatment strategies for glaucoma are individualized to achieve the greatest lowering of the intraocular pressure with the least amount of risk to the individual’s eyesight and well-being. Commonly, in the United States, topical medications are used as a first line of treatment. In many situations, multiple medications are used in an attempt to achieve the desired pressure level. Unfortunately, there can be difficulties with compliance, cost and side effects with many of these medications. Because of these and other reasons laser therapy (SLT) is commonly substituted as a first line of therapy. There are many other alternative treatments available, but they have increasing potential risk.
Recently there have been further medical advances made with the goal of achieving better control of the intraocular pressure. Minimally invasive glaucoma surgical procedures, (MIGS) involve making surgical changes to the drainage area inside the eye. The iStent® trabecular micro-bypass stent is a surgical therapy for patients who have mild to moderate open angle glaucoma and who have previously been treated with topical medications and/or laser therapy.
The iStent® is an elective procedure. As your surgeon has discussed, the iStent® is potentially beneficial in helping to reduce the number of glaucoma medications with this surgery, and by being in place and working 24 hours per day. If you decide not to have the iStent®, other treatment options may be recommended and should be discussed with your physician to help ensure adequate control of your glaucoma.
The iStent Trabecular Micro-Bypass Stent Procedure
The goal of the procedure is to improve the outflow of fluid from your eyes. The iStent® helps to control the pressure in the eye and reduce the risk of future vision loss to glaucoma. After implantation, many patients are able to better control their eye pressure with fewer glaucoma medications.
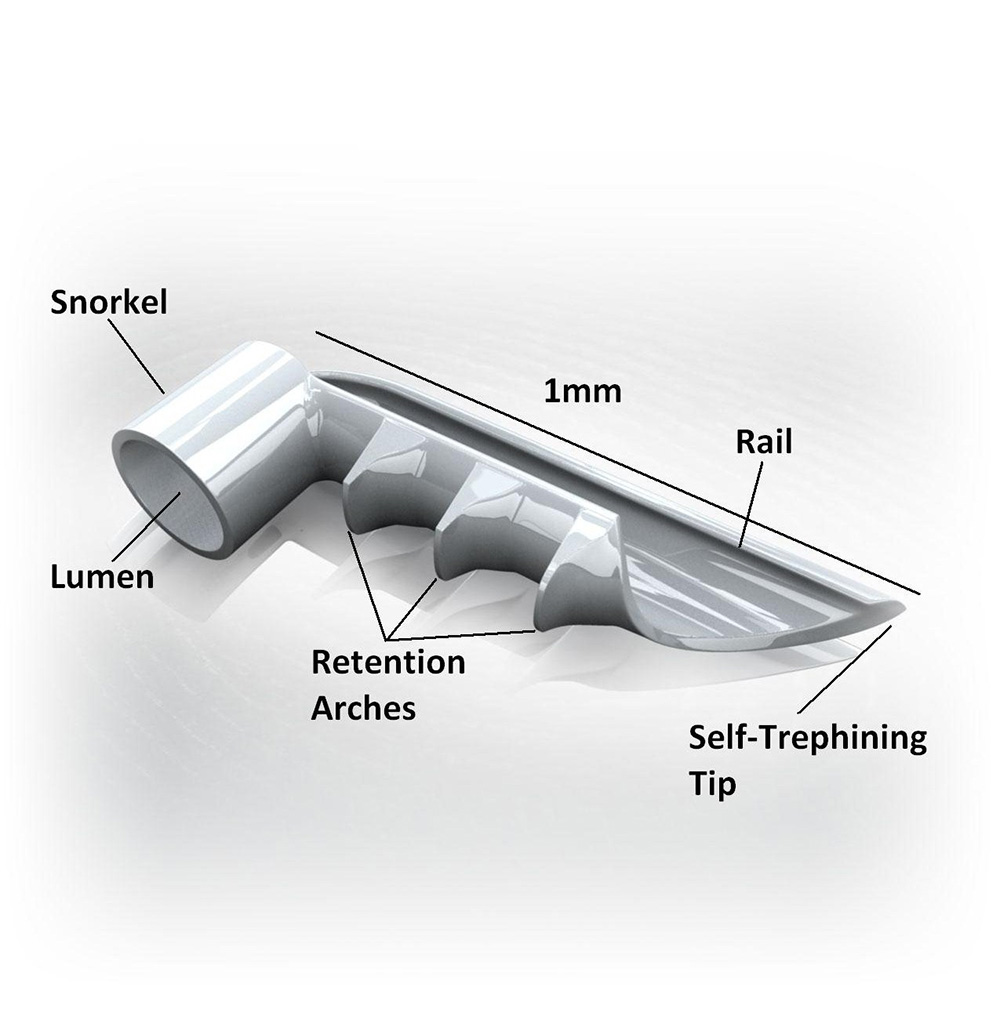
The iStent® is inserted through a small incision generally less than 2mm and can be performed under topical or local, regional anesthesia. The iStent® you will receive is performed in conjunction with your cataract surgery. Other risks potentially associated with anesthesia, depending upon the type of anesthesia used, include cardiac and respiratory problems, and in rare cases, death. All operations and procedures carry some level of risk and can result in complications, injury or even death from both known and unknown causes. The major risks of cataract surgery include, but are not limited to, infection, inflammation, injury to parts of the eye and nearby structures from anesthesia, the operation itself, or pieces of the lens that could remain in the eye following surgery, possible fluctuation in intraocular pressure, a detached retina or a drooping eyelid.
What are the Major Risks of the iStent?
As mentioned earlier, the iStent® has been demonstrated to successfully lower intraocular pressure in most cases when it is successfully implanted, but it may not necessarily stabilize your glaucoma. In some cases, it may not function well at all, even though it is properly placed. In addition, sometimes there can be complications that do not appear in the early post-operative period but may develop days, months or years later. You may need further treatment or surgery to treat those complications. As with any intraocular surgery, there is a risk of loss of vision, blindness, loss of the eye, as well as bleeding, infection, inflammation or injury to the eye or associated body structures.
